Choosing a health plan can be incredibly complicated — and choosing an ill-fitting plan for your employees, yourself, or your dependents can be costly. It’s a lot of pressure.
The best thing you can do to ensure the financial, physical, and mental well-being of your people is to learn as much as you can about your available options. One health plan option you might not be as familiar with is the narrow network plan. In this blog post, we’ll take a closer look at this type of plan to help you decide whether it might be right for your needs.
What Is a Narrow Network Health Plan?
Narrow networks are not necessarily all that new. Since the Affordable Care Act (ACA) was enacted in 2010, narrow network health plans — and even ultra-narrow network health plans — have been a popular choice among the self-insured; they accounted for about 72% of plans offered through the ACA exchanges in 2019. What is new is that these types of plans have been growing in popularity as an option for those in group plans.
What exactly constitutes a narrow network health plan? First, the term narrow refers to the fact that narrow network health insurance plans limit coverage to a select group of physicians, specialists, and hospitals. These plans are offered by traditional insurance providers — they aren’t a completely separate network, but they offer a narrower slice of coverage of what might be included in a traditional plan.
The second part of the term, network, refers to the fact that providers within a narrow network plan are typically chosen specifically because they already have strong working relationships with other in-network providers. They usually have a proven record of higher-measured quality and better outcomes for patients. This can be seen as a strength of narrow network health insurance plans — although provider options are fewer, those networks can result in better patient care.
Why Do People Opt for Narrow Network Health Plans?
Narrow network health plans are intentionally designed to be more affordable than traditional networks for just about everyone involved: insurance carriers, healthcare providers, employers, and employees.
Insurance companies offer narrow network plans as a cost-mitigation strategy: Providers within narrow networks typically accept lower reimbursement rates than out-of-network providers. These savings are passed on to employers (in the form of lower premiums), which explains why so many companies now offer these plans to their employees. This results in more affordable coverage for plan members — with a few caveats that we’ll discuss later.
Other benefits for narrow network health plan members can include free health coaching and live video services, which plan members can use to get answers from in-network providers without ever setting foot in a doctor’s office.
The Differences Between HMOs and Narrow Networks
The overall setup of narrow network healthcare plans is similar to that of an HMO, or health maintenance organization. Plan members are limited to a select number of healthcare providers, but this means they enjoy lower premiums and out-of-pocket expenses.
However, there are two key differences between HMOs and narrow network health plans. One difference (which is a benefit for plan members) is that narrow network health plans do not require patients to get referrals to see in-network specialists. This saves patients anywhere from $15 to $50-plus in copay costs each time they need to see a specialist, which adds up over time.
The other main difference is that narrow networks do not provide coverage for out-of-network providers, while HMOs typically provide some coverage. So when patients need to see providers who might not be associated with the narrow network, it can be extremely costly. Traditional plans — and HMOs — usually offer higher negotiated rates for out-of-network providers.
Narrow Networks and Out-of-Pocket Expenses
This brings us to some important considerations regarding narrow network healthcare: Are narrow network health plans actually more affordable when you factor in the potential cost of out-of-network providers? What is the likelihood that a narrow network plan member might incur some of these out-of-pocket costs — and what are their options if they cannot afford to pay them?
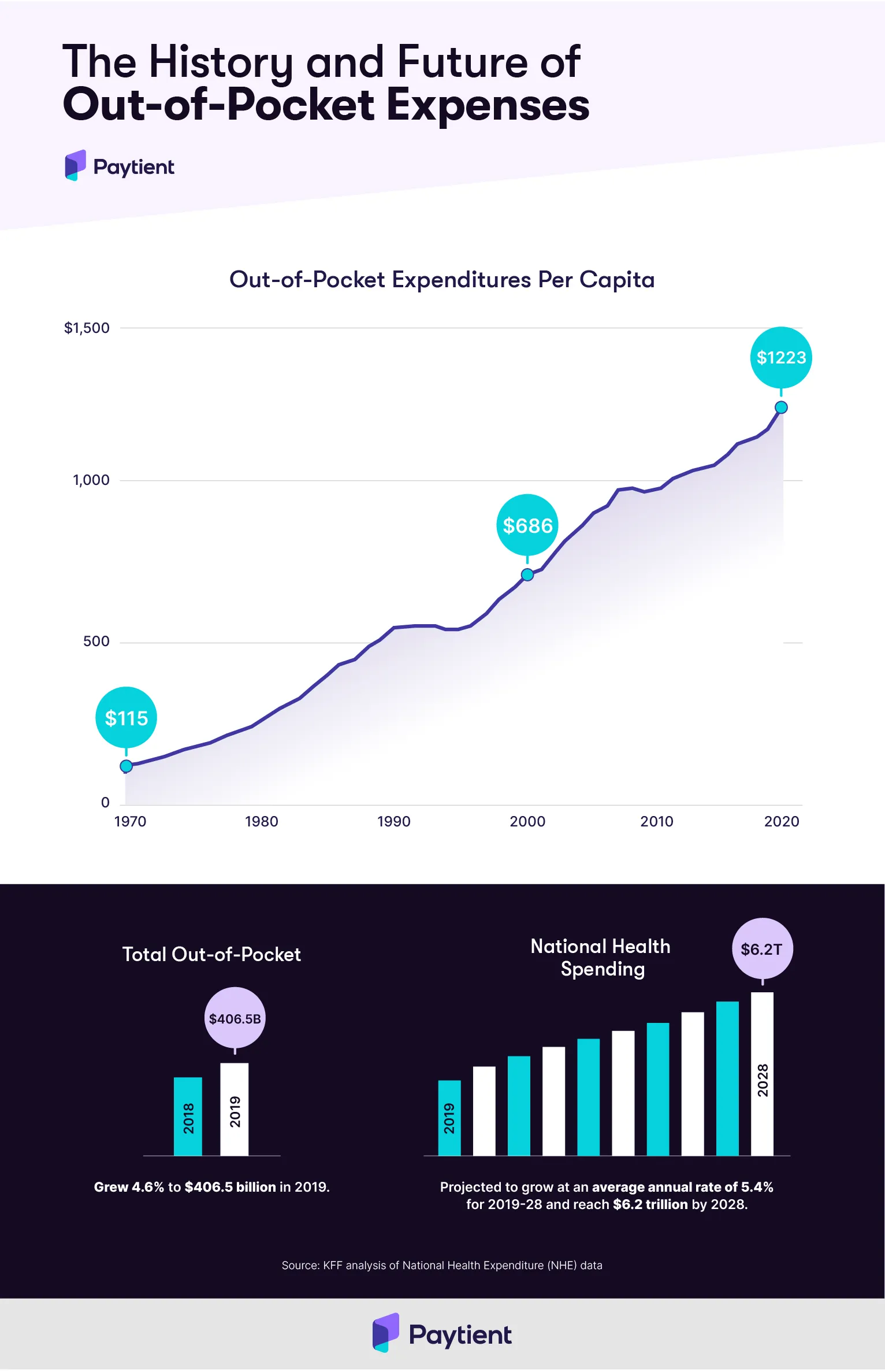
These are important questions to ask, but they are difficult to answer broadly. Employers looking to save on premiums might feel torn between being able to offer a more affordable plan (more affordable to them as the employer, and to their employees) and putting their employees in financially difficult situations if they do need out-of-network care.
Employers and employees need to know that out-of-network care is not a rare or fringe scenario for narrow network health plan members. Narrow network heath insurance plan members should prepare for the possibility of needing some out-of-network care, and ideally, will budget to be able to absorb that cost.
Depending on employees’ individual circumstances and needs, will vary widely from person to person. When choosing between a narrow and broader healthcare plan for your team, you’ll need to carefully weigh which is more beneficial to your group: There is no “right” answer, but there are ways to make whichever plan you choose work for more of your people.
Filling Gaps With Paytient
Offering Paytient as a benefit to your employees can help reduce their financial risk — regardless of the healthcare plan they have. Paytient enables employees to pay medical, dental, pharmacy, vision, or veterinary bills over time via post-tax, payroll-deducted, interest-free payments.
If you choose to offer a narrow network health insurance plan, Paytient can help plan members cover potential out-of-pocket costs — including charges from seeing out-of-network providers. This creates a rare win-win-win in the world of healthcare: Providers are paid at the time of service, employees can better access and afford care, and employers/health plans increase participation in lower-cost health plan designs.
If you decide to keep a broader market plan, Paytient can still add value: You can provide team members with peace of mind knowing they’ll be able to afford their care in full — and pay for it on whatever timeline fits with their finances. For more information on this, check out our blog post on.




.webp)